Myelodysplastic syndromes (MDS)
Myelodysplastic syndromes (MDS) are a group of conditions where your bone marrow does not work properly and makes faulty blood cells. MDS is a type of blood cancer.

What is MDS?
MDS is a type of blood cancer that affects your bone marrow and blood cells. Learn about what MDS is, what causes it and the different types of MDS.
MDS explained

Prognosis for MDS
The way MDS develops over time varies from person to person. Read about how MDS develops and what can affect your prognosis.
MDS prognosis

MDS symptoms
The main symptoms of MDS are caused by having low levels of healthy blood cells. Symptoms vary from person to person, depending on which blood cells are affected.
Common MDS symptoms
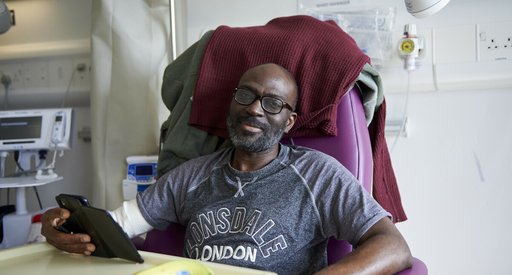
Treatment and side effects
Your hospital team will recommend the best treatment for you and help you with any side effects from your treatment.
Read about treatment

Tests for MDS
If your doctor thinks you might have MDS, they'll do some tests to find out more. After diagnosis you'll have tests to monitor the MDS and to check if any treatment is working.
Tests you may need

Active monitoring (watch and wait)
Some people with MDS don't need treatment straight away. If you don't need treatment, you'll go on active monitoring (watch and wait).
Active monitoring for MDS

Living well with MDS
Finding out you have MDS can be a big shock. Find out where to get support, and things you can do to help yourself.
Looking after yourself

Order your free guide to MDS
People with MDS helped us create this booklet, to help you understand what to expect and how to live well with MDS.
Get your free copy
This information has been accredited with the PIF TICK, the UK's only quality mark for trusted health information.
Many thanks to consultant haematologists Dr Daniel Wiseman and Dr Pramila Krishnamurthy for checking the medical accuracy of our MDS information.
